Just one decade ago, cases of epilepsy and Parkinson’s disease were untreatable, as were most cerebral injuries, and spinal or brain tumours, as well as muscular dystonia. Now, the Republican Scientific and Practical Centre of Neurology and Neurosurgery is finding new treatments, giving hope were none existed before.
“Neurosurgery has always been considered one of the most complicated branches of medicine, attracting the most dedicated, erudite and courageous experts,” underlines Ryshard Sidorovich, the Director of the Republican Scientific and Practical Centre of Neurology and Neurosurgery.
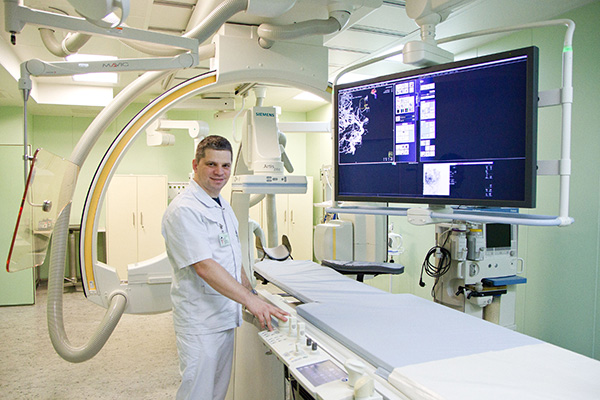
In the angiography room, a monitor shows a brain scan; vascular dilations are clearly visible. “There are multiple aneurisms,” explains Yevgeny Kisurin, who heads the angiography room. “The walls are very thin and may rupture at any time. The patient only has a 50-50 chance of survival, as any increase in blood pressure, from stress or physical activity, could cause a haemorrhage.”
Outstanding actor Andrey Mironov died following such a diagnosis but, today, patients are offered new treatments to alleviate risk. Using x-ray equipment, the doctor runs a micro-instrument through the femoral artery of the 61-year-old, filling the aneurysm with micro-spirals. This endovascular method significantly reduces the risk of rupture. In 2012, the centre conducted 134 similar surgeries, and completed 300 in 2015, of which 130 ‘neutralised’ aneurysms.
In the same room, the doctors ‘remove’ arteriovenous malformations of arteries and veins, since these can lead to haemorrhages and epileptic seizure. Alexey, 29, recently underwent surgery to remove dangerous ‘glomus’ from his circulation. Just 7 years ago, doctors would have been powerless, lacking the technology to operate so deeply in the brain.
Mikhail Talabaev, who heads the children’s department of the centre, comments, “17 years ago, when I began work in children’s neurosurgery, I admit that I felt frustration at seeing children in grave condition. Today, almost all of our patients leave fit and well, even helping carry their belongings. Over the last 5 years, we’ve mastered surgery not only on new-borns (aged up to 28 days), but from the first hours of life (one pathology requires neurosurgery immediately). Babies lack the protection which comes with age, leaving their spinal cord vulnerable, and with increased threat of infection, meningitis and death, so we operate immediately.”
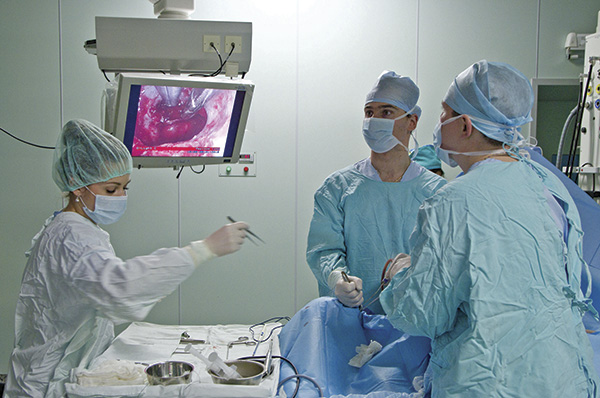
Two years ago, doctors at the centre began to remove tumours in the brain stem and other functionally significant regions of the brain, such as those responsible for the work of the lungs and heart, and for movement. Any error can cause irreversible neurologic damage; it’s incredibly fine work.
In determining the success of surgery, the priority isn’t just the removal of a growth, but survival with reasonable quality of life. Modern equipment helps to achieve this. Intraoperative neurophysiological monitoring helps trace the vital functions of an organism, guiding doctors in using instruments. The positioning station visualises tumours in 3D, helping immensely.
The Republican Scientific and Practical Centre of Neurology and Neurosurgery treats children not only from Belarus, but from Russia, Ukraine, Latvia, Georgia and other countries.
Recently, we operated on a 10-year-old boy from Ukraine, as hospitals in Uzhgorod and Kharkov felt unable to remove his tumour of the cerebellum. Our neurosurgeons decided to help, while admitting that recovery would have been far quicker if the child had been brought several months earlier.
Patients with Parkinson’s disease, generalized muscular dystonia, essential tremors, or severe pain syndromes (where even strong analgesics don’t bring relief) now have the option of neuro-modulation. This involves the implantation of a small neuro-stimulator, whose electrodes connect to the necessary region of the brain or spinal cord, providing an electric impulse. Every year, the centre carries out up to 30 such implantations, explains Candidate of Medical Sciences Vladimir Rerekhov, a neurosurgeon at Neurosurgery Department #1.
He explains, “As the device costs nearly $20,000, the doctors’ council decides on each patient case. Taking into account direct and indirect expenses, implantation is repaid within 4-5 years.” Patients are able to return to work, and medication expenses are halved or even reduced three-fold. People are more likely to avoid relapse and some manage without disability support or social workers.
Among those who have returned to normal living is a 7-year-old boy. His illness caused his body to make chaotic, spontaneous movements, all the time. After implantation of the neuro-stimulator, he began attending school and is doing well.
This year, experts are planning on treating severe, drug-resistant forms of epilepsy, using a similar method; in fact, not everywhere in Europe is yet using this technology.
By Alla Martinkevich
Facts
In November 2012, following a state investment programme, reconstruction was completed on the clinical building and a new surgical wing opened for the Republican Scientific and Practical Centre of Neurology and Neurosurgery (based on the Belarusian State Institute of Physiotherapy, created in 1924). Five years later, it was renamed as the Belarusian Science and Research Institute of Neurology and Neurosurgery. In 2005, it was reorganized as the Republican Scientific and Practical Centre of Neurology and Neurosurgery.